Remote Patient Monitoring Research
/Remote Patient Monitoring via Smartphone
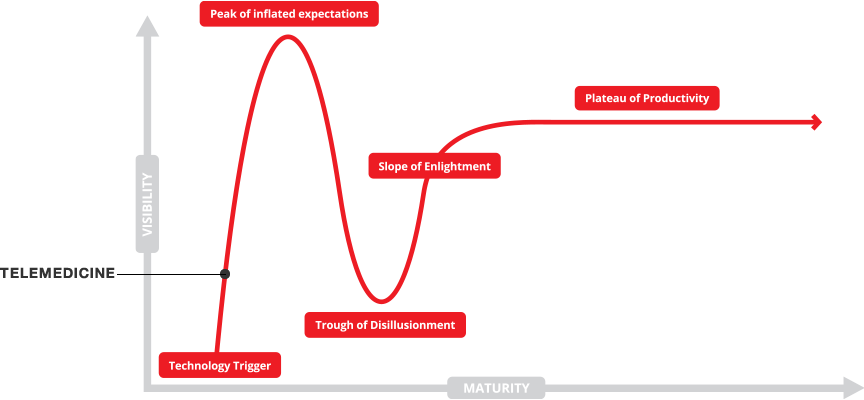
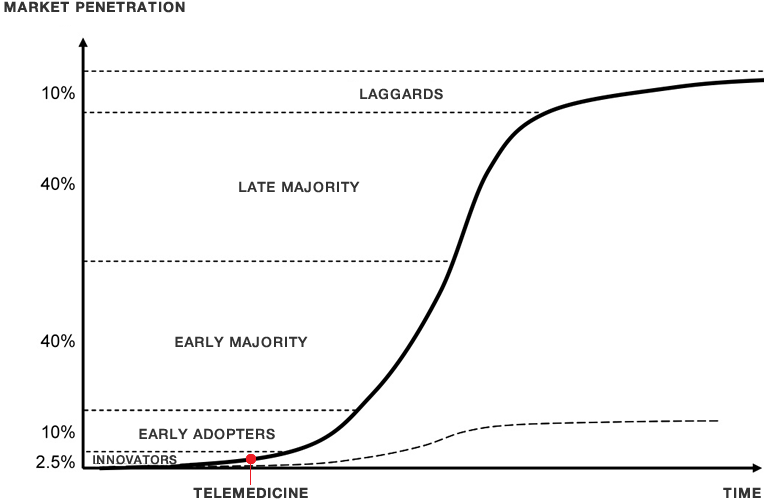
Telehealth is finally beginning to show real adoption with the move to outcome based care.
Any number of virtual care platforms have now thrown their hat in the ring to attempt to make patient communications as easy as regular calls.
Smartphone monitoring seems like a good option for physicians and patients alike. The literature on smartphone monitoring is limited, but it shows potential for clinical use.
In a recent study by Dalla Pozza et al. (2017), the researchers explored patient monitoring after treatment, which asked their patients to take photos of post-op procedure as they were instructed by their surgeons. Patients were asked to send photos of the front and side views of their face to send to the surgeons.
Out of the original 57 in the sample, only fifty followed-up with post-operative photos.
The following procedures performed were:
- (32) Facelifts, platysmaplasty, submental lipectomy;
- (14) Upper and lower blerophaplasty;
- (11) Fat injections
After treatment, three patients experienced complications early on. The patient in the study still preferred the usual face to face consultation, but the researchers mention that most of their sample were older patients, and were not able to adapt to some applications used for the study.
A similar study also examined the use of patient monitoring via smartphone. Chee et al. (2016) focused more on laser resurfacing on the dermatological aspect of it. Their study provided insight on the patient’s use of smartphone monitoring. There were 123 patients in the study, and having done the procedure around 12% had adverse events after it. Due to the complications, the dermatologist treated them the day after. Numbers dwindled as only a few answered the follow-up survey leaving only a few to report the smartphone review had good effects on them.
According to the authors, 95% out of the 24 who completed their survey felt at ease with the teledermatology process.
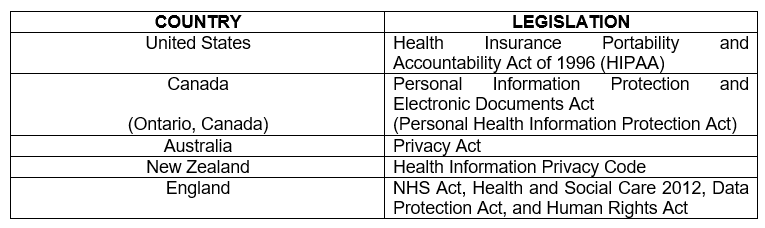
There is the risk of violating HIPAA and HITECH. In the first study, the researchers mention that limitation as patients may not have a HIPAA-compliant smartphone to send images or details of their condition. In this case, physicians have the responsibility to make sure their images are secure. In the second study, patients were wary with sharing their photos as well.
To learn more you might take a look at the scores from the KLAS 2017 Virtual Care Platform Report in which a dozen or so telehealth platforms (TruClinic, American Wellness, InTouch, etc.) were scored across a number of criteria.